The Road to Recovery in VR
It’s always been hard to watch your patients fight for mobility, month after month, often to make painfully few gains. So, you’ve become a master of both enthusiastic cheerleading and managing expectations – including your own.
And that cautious optimism was how you approached the incorporation of Virtual Reality into your physiotherapy rehabilitation practice. Muscles are resilient and the human brain is smart, but there are limits. Or so you thought.
Your most inspiring patient, let’s call her Jane Doe, was one of those people with a tragically unfair story behind her paralysis.
One rainy spring night, she was driving her children home from soccer practice, and the wrong combination of night lighting, slick pavement, and a drunk driver stole her mobility. She counts herself lucky that she was the only passenger hurt. But she still has two children to look after. To her, it’s not just her ability to walk she needs back; Jane wants to pick up her daughter, kick a ball with her son, and dance with her husband.
You can motivate Jane, but you know she’s got a long road ahead – one that probably doesn’t end with her life going back to the way it was before.

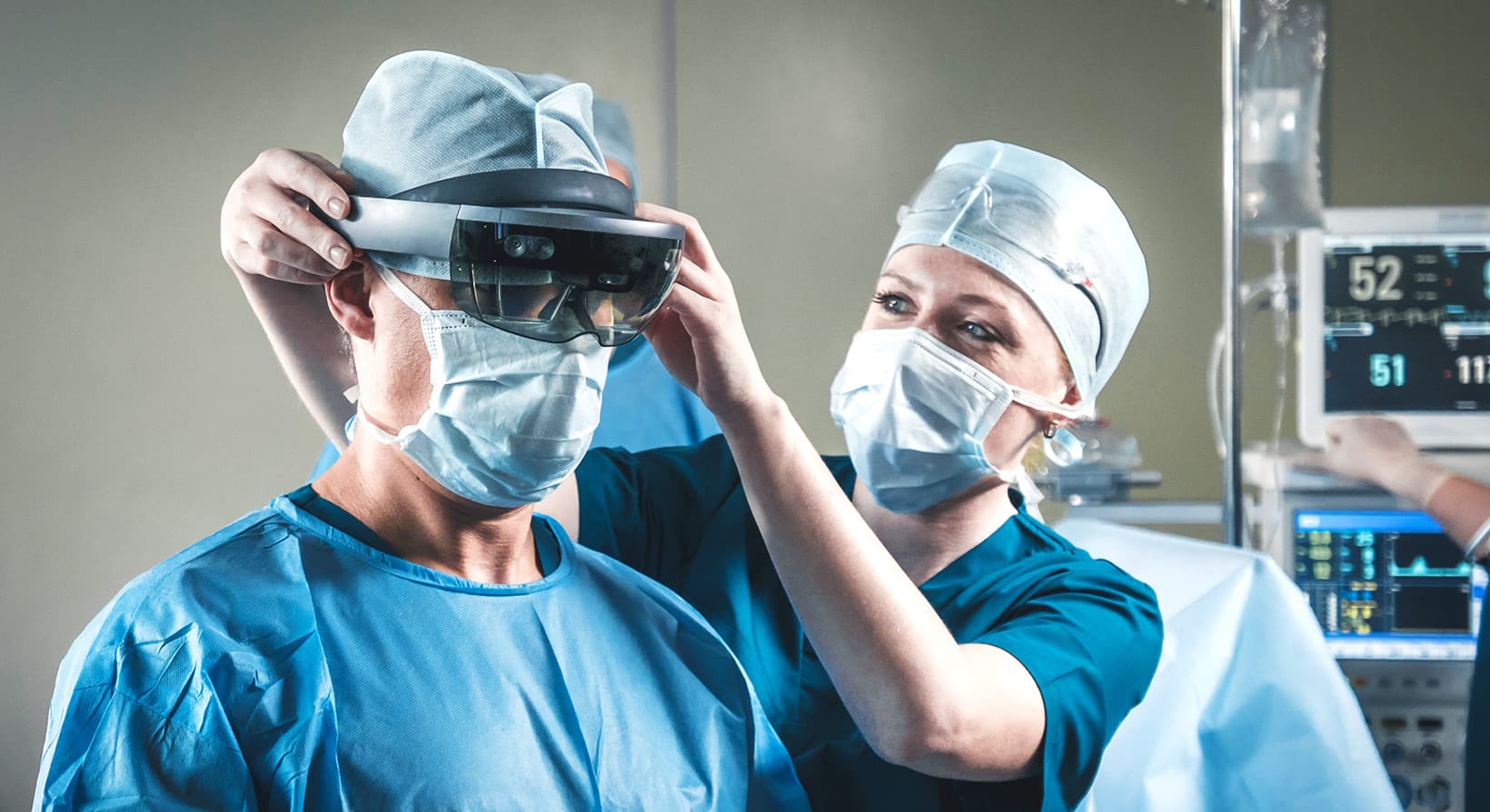
Image Credit: zinkevych / Adobe Stock
When you first learned about VR for rehabilitation, Jane Doe was a new patient. You’d read a journal article about how VR could be used as a learning tool to help wheelchair users adapt to a new lifestyle. With a headset and a joystick, the user could practice navigating a mall or a busy sidewalk. VR could also train users to cook, clean, or perform household tasks, giving him or her the confidence to transition back to independence.
You decided to start with Jane, a patient who needed your help more than most. She embraced the idea, but she was still heartbroken, still lacked motivation, and progress was slow.
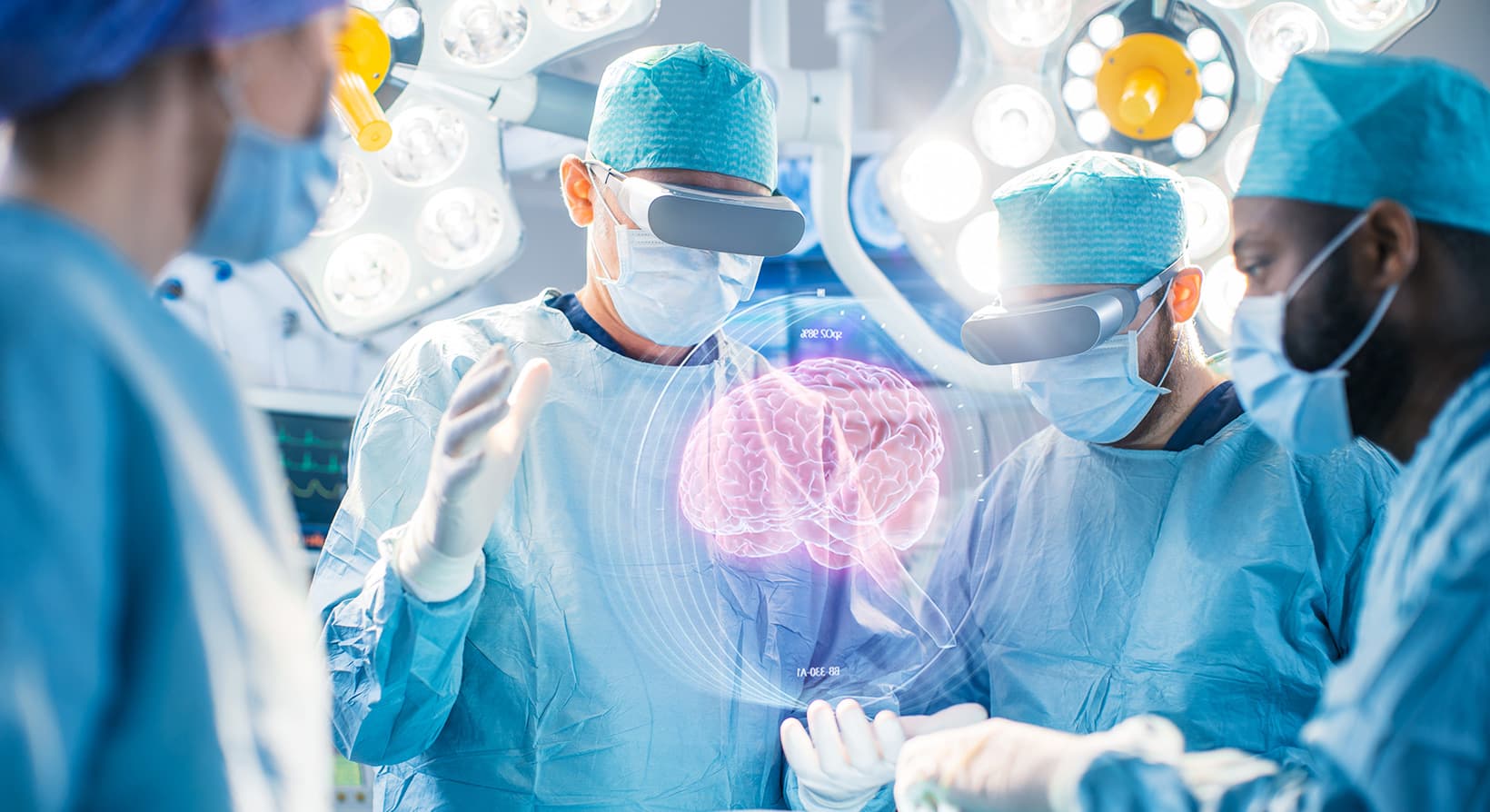
Then you heard about something much more interesting. VR was showing potential in improving motor skills and aiding in muscle recovery. And combined with a Brain Machine Interface (or BMI) the impossible was happening for paralyzed patients. Cyborgs had arrived.
Mechanical exoskeletons, powered by a patient’s own brain activity, would take the place of inactive nerves and muscles. Sensations were rekindled. It seemed too good to be true, but you knew it was real.
You mulled it over for several weeks, but eventually you decided to share a few articles with Jane, and a few other patients. Cyborg technology wasn’t something your clinic could adopt in the near future, but you wanted to show your patients what will be possible, in time.
Your clinic continued purchasing more VR software, exploring new hardware products like treadmills and haptic suits. You could see how all this Extended Reality technology is going to change everything.

Image Credit: WavebreakmediaMicro / Adobe Stock
Another patient you’ve initiated in VR is stroke survivor John Smith – also not his real name of course. His progress is making you smile too. He had just retired, was beginning to enjoy hosting his grandchildren for summer visits and building a small carpentry business in his garage. His life was good, and he deserved more than just basic mobility.
While you watch John work his way back from a massive stroke, you’re also witnessing him enjoying his first stroll along a beach in Bali.
VR has given your patients more than just a new tool in the battle to win back their bodies. For the individuals who need it – and they are many – the simple wellness benefit of sitting in a meadow or walking across a glacier is real, and it is powerful.
If someone had pulled your student self aside in the hall after a kinesiology class and said that you’d one day be using Virtual Reality as a therapeutic tool, you would have laughed out loud.
So today, you’re wearing that smile, but for a different reason.
At Stambol, we delight in watching how XR technology can make our world a better place, one life at a time. Ask us how we can connect your health care or wellness practice to the world of VR and AR.
Feature Image Credit: Sergey Ryzhov / Adobe Stock